Navigating Dyspraxia and ADHD: A Compassionate UK Guide
A clear guide to dyspraxia and ADHD in the UK. Understand symptoms, diagnosis, and support for adults and children.
It's easy to see why Dyspraxia and ADHD get mixed up. They're both neurodevelopmental conditions, and they often show up together, creating a unique and sometimes confusing set of challenges. At their core, though, they're quite different. ADHD primarily affects executive functions—things like focus, impulse control, and emotional regulation. Dyspraxia, also known as Developmental Coordination Disorder (DCD), impacts the brain's ability to plan and carry out physical movements.
Because they can look so similar on the surface and so many people have both, understanding where they overlap and where they diverge is the first crucial step to getting the right diagnosis and support.
ADHD vs Dyspraxia At a Glance
To quickly get a handle on the main differences, this table breaks down their primary characteristics.
| Characteristic | Primarily Associated with ADHD | Primarily Associated with Dyspraxia (DCD) |
|---|---|---|
| Core Challenge | Difficulty with focus, impulse control, and hyperactivity. A persistent pattern of inattention and/or hyperactivity-impulsivity. | Difficulty with motor coordination, planning, and executing movements. |
| Common Signs | Procrastination, forgetfulness, losing things, restlessness, trouble waiting your turn, interrupting others. | Clumsiness, poor handwriting, difficulty with sports, trouble with tasks requiring fine motor skills (e.g., tying shoelaces, using cutlery). |
| Impact on Organisation | Trouble organising tasks and activities, managing time, and planning ahead due to executive function deficits. | Difficulty with the physical act of organising—sequencing steps to tidy a room, arranging items on a desk. |
| Primary Brain Function Affected | Executive functions (working memory, inhibition, cognitive flexibility). | Motor planning (praxis) and sensory processing. |
While this table highlights the key distinctions, remember that in real life, the lines are often blurred, especially when someone has both conditions.
Untangling the Overlap Between Dyspraxia and ADHD
Think of ADHD and Dyspraxia as two distinct but overlapping circles. Each has its own set of core traits, but there’s a significant shared space in the middle where their symptoms can look almost identical.
At its heart, ADHD is a condition of self-regulation. It makes it tough to manage your attention, rein in your impulses, and keep your emotions on an even keel. Dyspraxia (DCD), on the other hand, is fundamentally a motor-planning issue. It’s about the brain’s struggle to process information and then tell the body how to perform a coordinated physical action.
This diagram helps visualise how the two conditions relate, showing where they stand apart and where their challenges intersect.
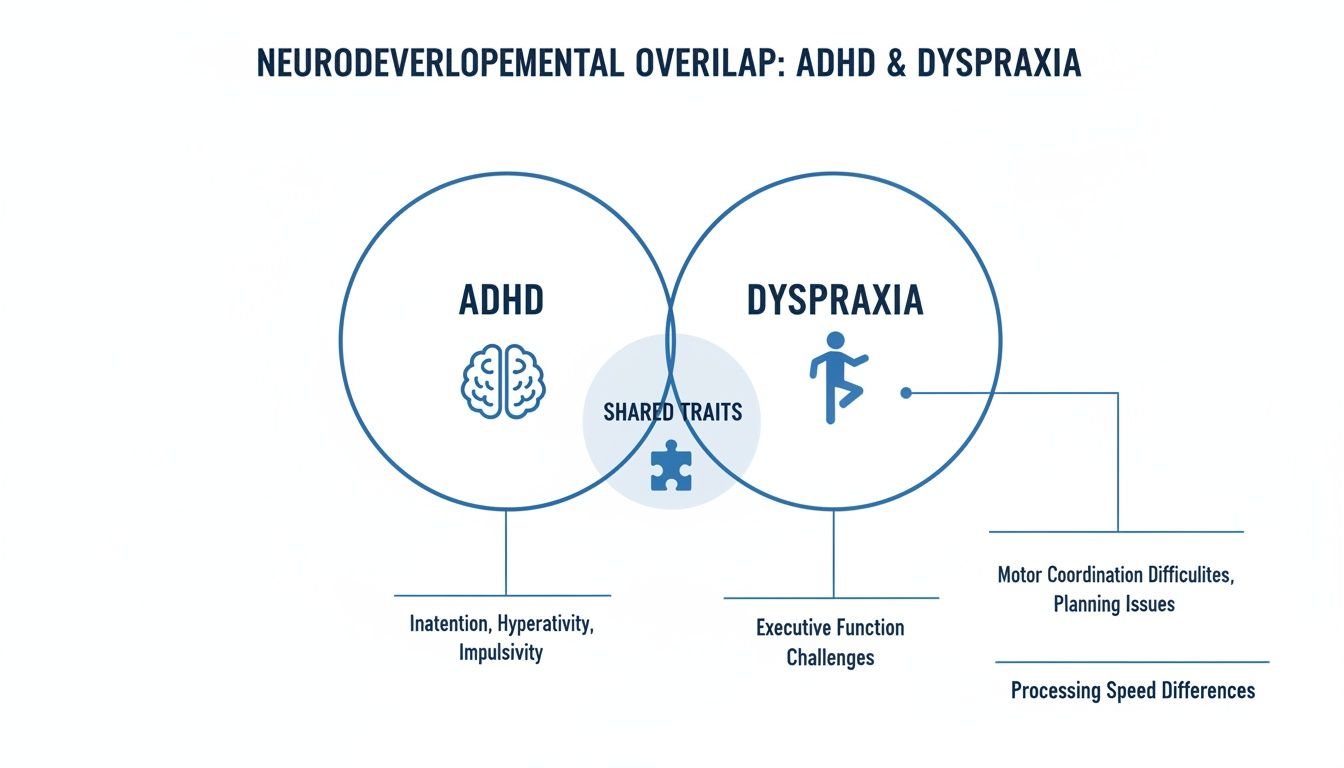
As you can see, even though one is rooted in executive function and the other in motor control, they meet in the middle on things like organisation and planning.
Why Do They Overlap So Often?
This high rate of co-occurrence isn’t just a coincidence—it points to shared neurological roots. The link is especially strong in the UK, where studies have found that up to 89% of people with ADHD also have DCD. Going the other way, around 50% of those with DCD also meet the criteria for ADHD.
This isn't just a statistic; it shows a powerful, two-way relationship between the conditions that can complicate daily life and really calls for an integrated approach to diagnosis. When they exist together, one condition can easily amplify the challenges of the other.
"ADHD affects executive function, which affects attention control, mood, motivation, short-term memory and your ability to prioritise and plan. Dyspraxia means that things that require dexterity are harder for me. Together they affect pretty much everything to do with moving through the world."
For instance, the executive dysfunction from ADHD can make it almost impossible to start a task. Then, the motor-planning difficulties from dyspraxia can make it physically frustrating to complete it. This double-whammy impacts everything from handwriting and sports to organising a workspace or simply managing your time.
Seeking a Combined Diagnosis
Because the symptoms are so tangled, getting an accurate picture often means finding a specialist who understands both conditions and how they interact. A comprehensive assessment is key.
A clinician experienced with co-occurring ADHD and Dyspraxia can tease apart the symptoms to identify the root cause of specific difficulties. This is absolutely vital for creating a support plan that actually works. You can explore a variety of providers, including the Autism and ADHD Diagnostic Centre, which specialises in assessments for co-occurring conditions. Knowing what to expect during the process can make all the difference, helping you feel more prepared and confident in your journey.
Recognising Shared Symptoms and Key Differences

Trying to tell dyspraxia and ADHD apart can feel like navigating through a thick fog. Many of their challenges meet and mingle, creating a confusing picture that makes it tough to work out what’s really going on.
So many of the daily struggles – like disorganisation, chaotic timekeeping, and feeling emotionally overwhelmed – are common to both. Getting your head around this shared ground is the first step to untangling which condition, or which combination of traits, best describes your experience.
Exploring the Overlapping Challenges
At a glance, the day-to-day frustrations of dyspraxia and ADHD can look identical. Someone might be constantly losing their keys, fighting to meet deadlines, or feel completely swamped by a simple set of instructions. But the reason for that struggle is often worlds apart.
Let’s take the classic example of a messy desk.
- For someone with ADHD: The mess is often a direct result of executive dysfunction. They might struggle with object permanence (if I can't see it, it doesn't exist), find it impossible to start the task of tidying, or get sidetracked halfway through. The mental energy needed to sort and put things away is just enormous.
- For someone with dyspraxia: The chaos might come from poor spatial awareness and difficulty with sequencing. They could struggle to visualise how to organise the space or find the physical act of arranging items awkward and frustrating. Their brain is having a hard time creating and then executing the motor plan for tidying up.
It’s a subtle distinction, but a critical one. In both cases, the desk is a mess, but the underlying neurological engine driving the chaos is different. This same principle applies to a whole host of shared symptoms.
Think of it like two people arriving late for a meeting. One was late because they lost all track of time and couldn’t prioritise getting out the door (an ADHD-style executive function issue). The other was late because they fumbled with their coat, struggled to get the key in the lock, and found it hard to navigate the physical route (a dyspraxia-style motor planning issue). Same result, very different cause.
Drawing Clear Lines in the Sand
While the overlap is significant, some core features are unique to each condition. Pinpointing these key differences is vital for getting an accurate diagnosis and, more importantly, the right kind of support.
ADHD is primarily about challenges with attention and self-regulation. Its classic traits are rooted in the brain's executive control centre.
Classic ADHD Traits Include:
- Persistent Inattention: Finding it hard to stay focused, being easily sidetracked, and being forgetful in daily life.
- Hyperactivity: An internal feeling of restlessness, fidgeting, not being able to stay seated, or talking excessively.
- Impulsivity: Acting on a whim without thinking, interrupting people, and finding it difficult to wait your turn.
In contrast, dyspraxia (DCD) is defined by its impact on motor skills and physical coordination. These challenges come from the brain's ability to plan, sequence, and carry out movements.
Classic Dyspraxia (DCD) Traits Include:
- Poor Motor Skills: General clumsiness, difficulty with fine motor tasks like handwriting or using a knife and fork, and struggles with bigger movements like catching a ball.
- Balance and Proprioception Issues: An unsteady walk, bumping into things, and a poor sense of where your body is in space.
- Difficulty Learning Physical Sequences: Struggling to learn multi-step movements like tying shoelaces, dancing, or driving a car.
By carefully mapping your own experiences against these distinct profiles, a clearer picture can start to take shape. This kind of self-reflection is an invaluable part of the journey, helping you to explain your specific challenges much more clearly when you eventually seek a professional assessment.
What It's Really Like to Live with Both ADHD and Dyspraxia
When you have both dyspraxia and ADHD, you're not just dealing with two separate lists of symptoms. You're living with a unique, often confusing, and compounding experience. The challenges of one condition have a knack for making the other one harder, creating a ripple effect that can touch almost every part of your life.
This isn't just about being a bit forgetful or clumsy. It’s about the very real, day-to-day impact of a brain that’s being pulled in two different directions at once. Getting your head around this dynamic is the first step toward understanding your own struggles and fighting for the support you actually need.
The Daily Compounding Effect
Let's put it into a real-world context. Imagine you’re trying to take notes in a university lecture. Your ADHD brain is fighting a constant battle to stay focused on the speaker, tune out the whispers a few rows back, and stop your mind from wandering off on a tangent. At the exact same time, your dyspraxia is making the simple act of writing quickly and legibly feel like a monumental, exhausting task.
One condition is sapping your mental energy, while the other is draining your physical coordination. The result? You walk out of the lecture feeling completely defeated, with a notebook full of half-finished sentences, convinced you’ve failed on two fronts. This is the reality of co-occurring conditions; the challenges don't just add up, they multiply the effort needed for everyday tasks.
Think about these common scenarios where dyspraxia and ADHD can create a perfect storm:
- At Work: The ADHD-driven struggle to prioritise tasks collides with the dyspraxic difficulty in planning the physical steps to get them done. A project can feel overwhelming before you've even started.
- Social Situations: ADHD can make it tough to follow the thread of a conversation without interrupting. Meanwhile, dyspraxia can throw your body language and spatial awareness off-kilter, making you feel awkward and clumsy in crowded spaces.
- At Home: The motivation to tidy a messy room might be nowhere to be found, thanks to ADHD. But even if a sudden burst of energy strikes, dyspraxia can make the physical act of sorting, organising, and putting things away feel hopelessly complex.
The Emotional and Psychological Toll
Living with this constant internal friction takes a serious toll on your self-esteem and mental health. When tasks that seem simple for others require a huge amount of effort from you, it's all too easy to start seeing yourself as a failure.
So many people with undiagnosed co-occurring conditions spend years, even decades, believing they are "lazy," "stupid," or "just not trying hard enough." This harsh internal monologue is often echoed by feedback from teachers, bosses, or even well-meaning family who just don't grasp the neurological reasons behind the struggles they see.
For many, getting a dual diagnosis is a genuine turning point. It provides a name and a reason for a lifetime of misunderstood challenges, finally replacing self-blame with self-awareness and compassion. It explains why some things just are harder for you.
This constant battle can also ramp up anxiety levels. The fear of making a mistake, dropping something, forgetting an important appointment, or saying the wrong thing can lead to pulling back from social situations and avoiding new experiences. This isn't a character flaw; it's a completely understandable response to navigating a world not designed for your brain.
Advocating for the Right Kind of Support
Recognising the combined impact of dyspraxia and ADHD is the first, most crucial step toward building a life where you can actually thrive. It means you can stop looking for single-issue solutions and start seeking support that addresses both your executive function and your motor coordination needs at the same time.
In practice, this might look like:
- Workplace Adjustments: Asking for speech-to-text software to get around handwriting difficulties (tackling the dyspraxia) and using project management tools to stay on top of deadlines (tackling the ADHD).
- Therapeutic Approaches: Working with an occupational therapist to develop practical motor skills and life hacks, while also partnering with an ADHD coach to build strategies for better focus and organisation.
- Personal Strategies: Finding a type of exercise that helps with ADHD focus but is also dyspraxia-friendly. Think running or swimming, which are less complex than a fast-paced team sport involving a ball.
Understanding that you aren't dealing with two separate problems but one interconnected experience is incredibly powerful. It gives you the language to explain your needs more clearly and seek out the integrated support that will help you navigate your work, studies, and social life with far more confidence.
Navigating Your UK Diagnostic Pathway

Trying to get a formal diagnosis for both dyspraxia and ADHD can feel like navigating a maze blindfolded. The UK offers a few different routes to get an assessment, and each comes with its own set of timelines, costs, and procedures. Getting your head around these options is the first real step towards clarity and support.
Your journey will almost always start in the same place: with your GP. Think of this appointment as the main gateway, whether you're heading down the NHS route or looking at private options.
It’s a good idea to go prepared. Before you see your doctor, jot down a list of your symptoms and, more importantly, some real-life examples of how they affect you day-to-day. Don't forget to include examples from your childhood if you can remember them. The clearer you are, the easier it is for your GP to grasp the whole picture.
The NHS Pathway Explained
The standard approach is for your GP to refer you to a local NHS neurodevelopmental service. The biggest plus here is obvious: it's free.
The major downside, however, is the waiting time. Let's be frank, the lists for adult ADHD and dyspraxia assessments can be painfully long. We’re often talking months, and in many parts of the country, several years. For a lot of people, that delay is a massive hurdle to getting the help they need.
The fact that dyspraxia and ADHD so often show up together just adds to the pressure. With an estimated 89% of people with ADHD in the UK also having signs of dyspraxia, the demand for comprehensive assessments is huge, but the services are stretched to their limits. This gap is glaring when you look at the numbers: while nearly 6% of adults say they have significant ADHD symptoms, only about 1.8% actually have a diagnosis.
Once your GP has made the referral, you’re in the queue. It's really important to manage your expectations at this point. The care can be fantastic, but the process itself is often a serious test of patience.
When you do finally get to the top of the list, you'll have a thorough assessment with a specialist, like a psychiatrist or clinical psychologist, who will look at everything to make a diagnosis.
Exploring the Private Assessment Route
If you can't face the long wait, going private is a much quicker alternative. Many people choose this route to get a diagnosis and start treatment in a matter of weeks or months, not years.
Of course, this means you're paying for the assessment yourself. Costs vary a lot from one clinic to another, so it’s essential to shop around. You can either approach a private clinic directly or ask your GP for a referral letter, as some providers still ask for one.
Key benefits of the private route include:
- Speed: The wait is often just a few weeks.
- Choice: You can pick your clinic and even your specialist, perhaps finding someone with particular expertise in co-occurring conditions.
- Flexibility: Many private providers now offer online assessments, which makes the whole process much more convenient.
After getting a private diagnosis, you might be able to set up a shared-care agreement. This is where your GP agrees to take over prescribing your medication based on the private specialist's recommendations, moving the ongoing cost back to the NHS.
Understanding Your Right to Choose
There's also a fantastic middle-ground option in England called NHS Right to Choose (RTC). This legislation gives you the right to choose where you have your NHS-funded assessment and treatment.
In practice, this means that if you're referred for an adult ADHD assessment, you can pick a qualified private provider that has an NHS contract, and the NHS foots the bill. Not every private clinic is part of this scheme, but many of the top ones are.
The RTC route is usually much faster than the standard NHS wait, though it can be a bit slower than paying privately. Essentially, it lets you tap into the speed of the private sector without the cost. To find out more, take a look at our detailed guide on the NHS Right to Choose pathway. It’s a powerful tool that puts you back in control of your healthcare journey.
Comparing NHS and Private Assessment Pathways
Choosing between the NHS, private, and Right to Choose pathways can feel overwhelming. To make it simpler, here’s a breakdown of what you can expect from each.
| Feature | NHS Pathway | Private Pathway | NHS Right to Choose |
|---|---|---|---|
| Cost | Free at the point of service | Self-funded (costs vary widely) | Free (funded by the NHS) |
| Waiting Time | Very long (months to several years) | Short (typically a few weeks to months) | Shorter than NHS (months, not years) |
| Choice of Provider | Limited to your local NHS trust | You choose any private clinic/specialist | You choose from a list of approved providers |
| Assessment Process | Comprehensive, but can be slow | Often faster and more flexible (e.g., online) | Uses the private provider's process |
| Post-Diagnosis Care | All follow-up and treatment via NHS | Can be self-funded or via a shared-care agreement | Follow-up and treatment funded by the NHS |
Ultimately, the 'best' path depends entirely on your personal circumstances—your finances, how urgently you need support, and where you live in the UK. Understanding these key differences is the first step in making an informed choice that's right for you.
Building Your Toolkit of Support Strategies
Getting a diagnosis of co-occurring dyspraxia and ADHD isn’t an endpoint; it’s actually the starting line for a more understanding, compassionate journey. This is the point where you shift from simply knowing about your challenges to actively managing them. Building a personal toolkit of strategies is all about discovering what works for your unique brain.
There's no magic bullet or one-size-fits-all solution here. A truly effective support plan will draw from different parts of your life, weaving together a safety net that tackles both the executive function hurdles of ADHD and the motor coordination difficulties of dyspraxia. This holistic approach empowers you to genuinely improve your day-to-day life, one practical step at a time.
Adjusting Your Environment for Success
It's often the simplest changes that pack the biggest punch. Instead of constantly trying to force your brain to fit the world, you can tweak your surroundings to better suit your brain. The goal is to reduce friction and make everyday tasks less of an uphill battle.
Take a look at your workspace or home. Small adjustments can do wonders to minimise sensory overload and streamline physical tasks, freeing up precious mental energy.
Practical Environmental Adjustments:
- Ergonomic Tools: Look into items that make physical tasks easier. This could be a vertical mouse, a specialised keyboard, or pens with comfortable grips to take the strain out of handwriting.
- Sensory-Friendly Spaces: For ADHD-related focus issues, a good pair of noise-cancelling headphones can be a lifesaver. For dyspraxia, make sure you have clear, uncluttered walkways to move around without constantly bumping into things.
- Visual Organisation Systems: Think clear storage boxes, colour-coded files, and a trusty label maker. When everything has a designated, visible home, it’s far easier to find things and much less overwhelming to tidy up.
These small modifications work together to create an environment that supports you rather than works against you—a powerful foundation for building other skills.
Finding the Right Therapeutic Support
While environmental changes help with the ‘what,’ therapeutic support gets to the ‘how.’ Working with the right professionals can equip you with specific skills to navigate the combined challenges of dyspraxia and ADHD, building both your competence and your confidence.
The trick is to find therapies that acknowledge the interplay between the two conditions. An approach that only targets ADHD’s executive function issues without considering dyspraxia’s motor challenges (or vice versa) is only going to be half-effective.
"I don’t expect everyone to be experts on dyspraxia or ADHD, but I’d like people to respect that it can mean my experience is different from theirs and what seems simple, helpful, important or fun to them might not be for me, or for everyone." - Maxine Roper, Author
One of the most effective supports is Occupational Therapy (OT). An occupational therapist is fantastic at helping you break down complex physical tasks into manageable steps, develop strategies to improve motor skills, and find practical workarounds for daily activities.
On top of that, Cognitive Behavioural Therapy (CBT), a common go-to for ADHD, can be incredibly helpful. It gives you the tools to challenge negative thought patterns, manage emotional ups and downs, and strengthen executive functions like planning and time management. When you can regulate your focus and emotions better, it becomes much easier to engage with and practise the motor skills you’re working on in OT.
Leveraging Technology as an Ally
Let's be honest, modern technology offers a huge array of tools that can act as an external hard drive for your brain. These aids can help bridge that frustrating gap between what you intend to do and what you actually do, which is often where people with co-occurring dyspraxia and ADHD get stuck.
Technological solutions can automate, simplify, or completely bypass tasks you find particularly difficult. This isn't "cheating"; it's simply working smarter.
Helpful Tech Tools Include:
- Speech-to-Text Software: This is a game-changer for anyone who finds the physical act of writing a struggle. Tools like Dragon or the built-in voice typing on your phone make getting thoughts onto the page faster and far less frustrating.
- Digital Planners and Reminders: Apps like Google Calendar, Todoist, or Trello can be your personal assistant—managing your schedule, pinging you with reminders, and helping you visualise tasks. This is a powerful aid for both ADHD-related time blindness and dyspraxic sequencing difficulties.
- Mind-Mapping Software: If you find linear note-taking a nightmare, mind-mapping tools let you organise your ideas visually, which can feel much more intuitive and natural.
Physical activity can also be a crucial part of your toolkit. For more ideas on how movement can support your brain, read our guide on effective exercises for ADHD, keeping in mind which activities feel most comfortable for your body. The ultimate aim is to build a customised plan that genuinely works for you, combining the strategies that make your daily life smoother and more manageable.
Frequently Asked Questions About Dyspraxia and ADHD

When you're trying to understand the connection between dyspraxia and ADHD, it’s only natural for questions to pop up. Let's tackle some of the most common ones we hear from adults, parents, and healthcare professionals.
These are the real-world queries that come up time and again, and my aim is to give you clear, practical answers that build on everything we've covered so far.
Can You Grow Out of Dyspraxia or ADHD?
In a word, no. Both conditions are lifelong neurodevelopmental profiles, not childhood phases you simply outgrow. Think of them as part of your fundamental wiring.
But that absolutely doesn't mean things can't get better. Over time, with the right strategies, therapies, and support systems, people learn to manage their challenges brilliantly. The difficulties might look different in adulthood compared to childhood, but the underlying neurotype is always there.
Is It Possible to Only Be Diagnosed with One at First?
Yes, and this happens all the time. It’s incredibly common for one condition to be spotted while the other remains hidden in plain sight for years.
Often, it's the more obvious symptoms—like the hyperactivity of ADHD—that lead to that first diagnosis. The quieter, overlapping traits, such as organisational struggles that could stem from either dyspraxia or ADHD, are easily overlooked or just lumped in with the initial diagnosis. This is exactly why a comprehensive assessment that looks for co-occurring conditions is so crucial.
It's not unusual for a dyspraxia diagnosis to come first, followed by an ADHD diagnosis years later, or vice-versa. Many people describe the second diagnosis as the final puzzle piece that makes their lifelong experiences finally make sense.
How Can I Support My Child with Both Conditions?
Supporting a child with both dyspraxia and ADHD is all about taking a patient, multi-layered approach. The best thing you can do is build a fantastic support team around them.
- Team up with their school: Work together to create an Individual Education Plan (IEP) or similar support document. It needs to address both their motor skill difficulties and their executive function challenges.
- Find an occupational therapist: They are brilliant at building practical motor skills—everything from handwriting to tying shoelaces—which gives a massive boost to a child’s independence and confidence.
- Consider a psychologist or ADHD coach: Someone who truly gets ADHD can help your child develop strategies for focus, organisation, and managing their emotions.
- Create structure at home: Predictable routines, visual aids like checklists, and breaking down tasks into tiny, achievable steps can make a world of difference.
Most importantly, celebrate their effort, not just the outcome. Acknowledging their hard work and small wins is one of the most powerful things you can do to build their self-esteem.
Do ADHD Medications Help Dyspraxia Symptoms?
This is a great question. ADHD medications are specifically designed to target the core symptoms of ADHD—inattention, impulsivity, and hyperactivity. They don't directly treat the motor coordination challenges that define dyspraxia.
However, there can be a really helpful knock-on effect. When medication helps someone manage their ADHD symptoms, their focus improves and they feel less restless. This newfound calm can make it much easier for them to engage with and benefit from things like occupational therapy. So, while it's not a direct fix for dyspraxia, it can be a vital part of a person's overall support plan.
Finding the right path to diagnosis is a critical step. At ADHD Private, we've created a free, UK-wide directory to help you compare over 85 private clinics, making it easier to find timely and suitable support. Explore your options for assessment and treatment at https://adhdprivate.co.uk.